
2021 in Review | No. 1 story: Hope for vaccines as COVID-19 attacks Nation
Navajo Times | Donovan Quintero
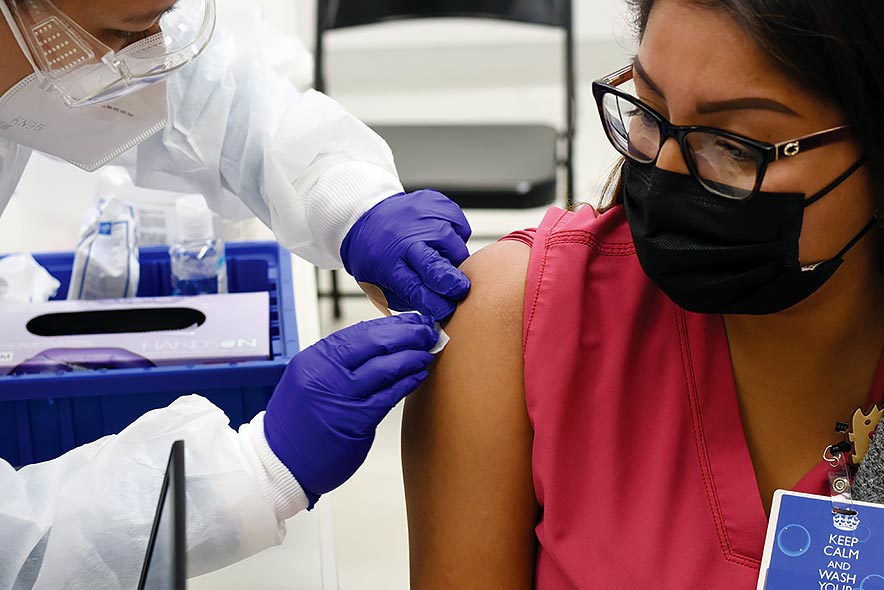
Shaiyaia Fowler, a medical assistant at Sage Memorial Hospital, gets the second dose of the Pfizer BioNTech vaccine on Tuesday, Jan. 5, 2021, in Ganado. Fowler and 164 colleagues who work with COVID-19 patients received their first dose on Dec. 12, 2020.
By Donovan Quintero, Krista Allen, and Rima Krisst
Navajo Times
WINDOW ROCK
More than a year after the first COVID-19 vaccine was authorized in the U.S., ch’osh doo yit’íinii, the coronavirus, continues to claim a record number of lives.
Top 10 Stories of 2021: No. 1
More than 5.4 million people worldwide (death toll surpassed 800,000 in the U.S. two weeks ago) have died from the disease since the pandemic began, according to John Hopkins University’s Coronavirus Resource Center.
Nearly two years into the pandemic that shows no sign of abating, it’s clear that the virus is one of the most common causes of death in the U.S., just behind heart disease and cancer, both of which kill about 600,000 Americans annually.
It might not seem like it now, but the coronavirus pandemic may end in 2022. To get there, more people must get vaccinated.
Even with the virus partially controlled by social distancing, masking, isolating sick and exposed people, closing places where people congregate in close quarters, a universal coronavirus vaccine is needed, Dr. Anthony Fauci, White House chief medical advisor, co-wrote in a paper titled “Universal Coronavirus Vaccines – An Urgent Need.”
Herd immunity
Four coronavirus outbreaks have occurred in the past 20 years: severe acute respiratory syndrome, or SARS, in 2003 and in 2004; Middle East respiratory syndrome, or MERS, in 2012; and now COVID-19.
The U.S. recently surpassed 50 million COVID-19 cases since the start of the pandemic, and Dec. 13, marked the anniversary of the first COVID-19 vaccination in the U.S. outside of clinical trials.
The virus, vaccines, and variants dominated headlines for a second year in 2021, as did the three “Ws” – wear a mask, wash your hands, watch your distance – even as millions of people took shots in their arms.
The first 3,900 doses of Pfizer-BioNTech’s COVID-19 vaccine arrived in mid-December 2020, and distribution to priority groups was launched within Navajo Area Indian Health Service units and tribal health organizations.
From there, the race was on to achieve herd immunity, which experts estimated would require 70% to 85% of the population vaccinated.
For the first few months of 2020, the Navajo Nation led the U.S. in vaccination rates – a significant feat.
However, one year later, 60% of the total population on Navajo is fully vaccinated, mirroring the national percentage of 61.2%, leaving more than a third of the population unvaccinated and vulnerable.
An estimated 80% or more of people nationwide getting hospitalized and dying from COVID-19 are unvaccinated.
Still, many people remain vaccine-hesitant, expressing concerns over the vaccines’ safety, long-term side effects, and efficacy.
COVID cases double
Navajo Times | Sharon Chischilly
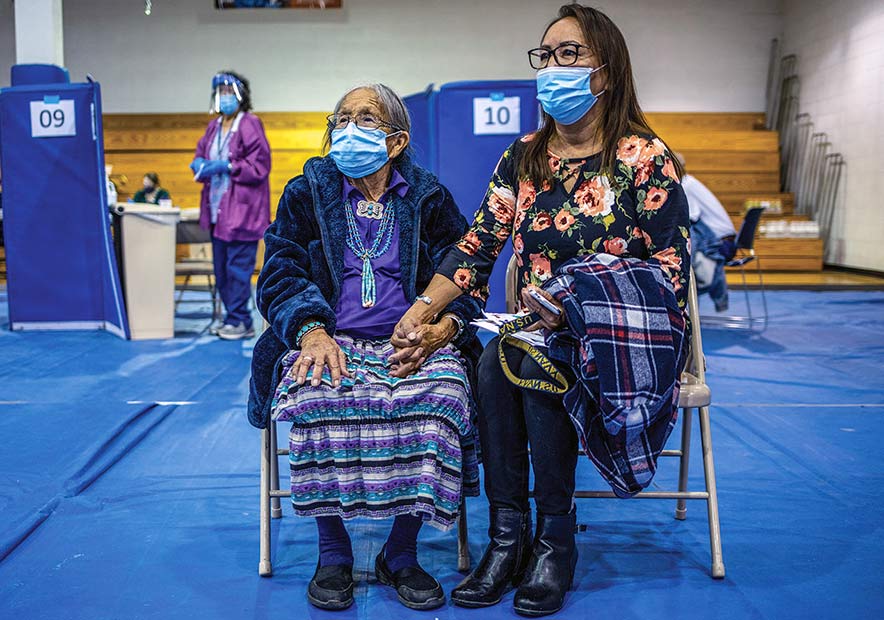
Ruth Armstrong (left) and Maxine Armstrong-Touchine wait after receiving their first Pfizer COVID-19 vaccine in the University of New Mexico-Gallup gymnasium Saturday, Jan. 30, 2021, in Gallup. Patients wait 15 minutes at the site to be monitored for any adverse reaction after being vaccinated.
A year ago, the number of deaths from COVID-19 on Navajo was 806, with 23,090 cases. Despite the rollout of the vaccine, the numbers have doubled in 2021.
The emergence of the more transmissible and infectious U.K. variant started wreaking havoc in late 2020 and became the dominant strain in the U.S. by the end of March.
Following a devastating holiday and winter surge heading into 2021, COVID-19 cases in the Nation steadily trended downward from February to July.
However, in February, health experts confirmed that people who have been vaccinated could still become infected and transmit the virus, which came as a shock to many who thought the vaccine protected against infection.
The good news was that scientific evidence shows vaccines are working to prevent severe illness and hospitalization, as demonstrated in clinical trials.
With virus cases easing up in the Southwest, Navajo businesses such as Navajo Nation Gaming Enterprise casinos started opening in April to 50% capacity.
The Indian Health Service on Dec. 17 reported that 338,299 COVID-19 doses had been administered, and 372,825 doses have been distributed. Overall, 2.5 million doses have been distributed to 11 IHS area offices throughout the country.
Since the coronavirus entered the Navajo Nation, 386,243 people tested for COVID-19. Of that number, 282,618 tested negative, and 45,518 tested positive.
The Navajo Department of Health reported on Dec. 26 that 1,583 Diné lost their lives to the virus.
To continue providing adequate services, Gallup Indian Medical Center implemented Crisis Standards of Care, which strained the hospital’s existing resources.
The purpose of the CSS is to treat the sickest patients first, according to an IHS Dec. 23 news release.
Because of the rise in COVID-19 cases, non-emergency patients may be delayed and appointments may be canceled.
Fauci says scientific evidence suggests that coronaviruses will emerge again in the future. He added that people infected naturally with SARS-CoV-2 could also be reinfected.
COVID-19 variants
Navajo Times | Sharon Chischilly
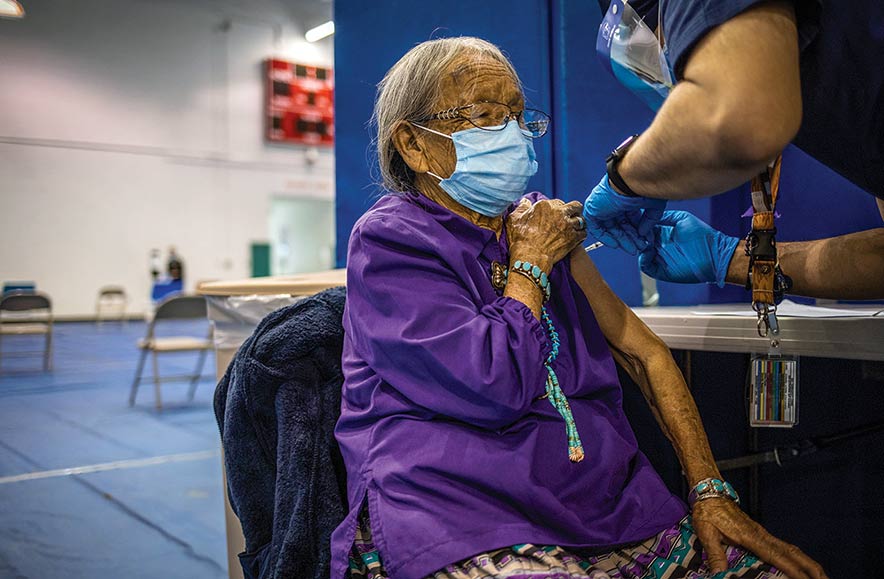
Ruth Armstrong, 88, receives her first Pfizer COVID-19 vaccine in the University of New Mexico-Gallup gymnasium during Gallup Indian Medical Center’s COVID-19 vaccination event Jan. 30 in Gallup.
The Omicron is piggybacking on the Delta variant that emerged in July.
Fauci said the Delta variant is twice as contagious as the UK even among the vaccinated who could be asymptomatic.
By mid-August, the Delta variant was dominant in the U.S., and it became clear we were not out of the woods yet.
Even with the Omicron – which was detected in Coconino County, according to the Tuba City Regional Health Care Corporation – currently affecting the country, getting vaccinated could end the pandemic.
Sixteen cases of the highly contagious Omicron variant have been reported in Arizona.
Communities will still see occasional outbreaks, but new drugs will be available that could take care of most cases, and hospitals will be able to handle the rest.
In the face of a possible significant COVID-19 surge, health experts doubled down on vaccination efforts and tightened up on COVID-19 safety precautions, including masking, avoiding large gatherings, and travel.
By Sept. 21, U.S. COVID-19 deaths surpassed the Spanish Flu pandemic milestone at 675,000 deaths.
As a throwback to 2020, as we approached fall and winter concerns prevailed over the challenge of flu season coupled with a surge in the virus.
The Delta variant also caused concern because it was sickening younger people, including children.
By the end of October, the U.S. Food and Drug Administration authorized the emergency use of the Pfizer COVID-19 vaccine for children 5 through 11 years of age.
In early November, the Mountain West region started seeing a significant surge, fueled by the Delta variant, casting uncertainty about what would transpire through the holidays and how that would impact travel and family gatherings.
We also learned about breakthrough infections among the vaccinated due to “waning immunity,” or the reduction in the vaccine’s immune protection due to declining antibody levels.
The efficacy of the Pfizer-BioNTech, Moderna, and Johnson & Johnson COVID-19 vaccines have initially been 95%, 94%, and 72%, respectively, but that declined dramatically within six months of getting the shots.
Then came booster shots to restore vaccine immunity that began to be administered to immunocompromised individuals and to the general population 18 and above by November.
By early December, the Delta surge filled Navajo Area hospitals with 65 chapters reporting “uncontrolled spread,” driving up the Intensive Care Unit occupancy rate to 100% and leading to patients being transported to hospitals out of state.
As the Navajo Nation rode its third COVID wave, health professionals prepared for the arrival of the new Omicron variant discovered in South Africa. Experts say this variant could evade vaccine protection because of its unprecedented number of mutations of the COVID-19 spike protein.
Changes in Diné Bikéyah
The Navajo Nation looks very different amid a pandemic that upended the rhythms of daily life.
People have lost precious time with family and friends, are forced to cancel travel plans, and miss milestone events like graduations and weddings.
For two years, the Navajo Nation fairs – that typically buoys Diné in every community – were muted.
And Upper and Lower Antelope Canyon, Tsébighánlini and Tsébii’ Hazdeestas-Tsé’ésdooltas were closed for 485 days because of the virus.
Yes, the Nation was hit hard by the pandemic. Some hospitals, school districts, and businesses across the Nation mandated vaccines, while others fought over whether to require masks inside a building or not.
Some school districts had in-person classes five days a week and no remote option. Many students, especially the younger ones, struggled to catch up.
Still, the Nation’s resilience is evident today despite the gray skies. You will see Diné as the only ones wearing masks in border towns like Farmington, Gallup and Page.
But amid the spikes and postponed parties, and lines at overburdened testing sites, there were glimmers of the Christmas season found across Nation, such as the Begay’s Kéeshmish Village in Many Farms brimming with determination and hope for a future without the virus.
Another pandemic holiday
While case numbers on Navajo trended downward through the Christmas holiday, infections in the U.S. overall are soaring and hospitalizations are increasing.
As reported by the New York Times data tracker, 543,415 cases were reported in the U.S. on Dec. 27, with a weekly average jumping 62.5% from from Dec. 19.
Omicron’s rise heralded another pandemic-tinged holiday for Diné, and many are experiencing lengthy separations from loved ones while others have been fortunate enough to come together more frequently.
As the Omicron’s variant spreads, health experts say the best defense against all virus variants is a full dose of a COVID-19 vaccine followed by a booster shot.
Since the first messenger RNA against the virus was authorized late last year, studies have shown that the unvaccinated are five times at greater risk of getting infected and 10 times greater risk of hospitalization or death from the virus than those who are fully vaccinated.
Over the Christmas weekend, major airlines canceled thousands of flights because of crew shortages due to Omicron infections, and virus-infected cruise ships were once again being denied port entry, leaving passengers stranded offshore.
On the bright side, Pfizer and Merck biopharmaceutical companies announced FDA approval of antiviral pills that can significantly reduce the severity of the illness when administered early after infection.
Still, last week the White House warned that it might take months before the pills are widely available due to the limited supply of the drugs.
In the meantime, health experts are recommending a switch from cloth masks to N95 masks better to protect oneself from Omicron.
As a public service, the Navajo Times is making all coverage of the coronavirus pandemic fully available on its website. Please support the Times by subscribing.
How to protect yourself and others.
Why masks work. Which masks are best.
Resources for coronavirus assistance








 Highway 264,
Highway 264, I-40, WB @ Winslow
I-40, WB @ Winslow